Abomics has long been the only pharmacogenetic test provider in Finland to include CYP1A2 gene variants in its pharmacogenetic panel. Until now, the evidence for the gene’s impact on drug efficacy and safety has been weak, which has resulted in Abomics assigning a low evidence level to the
pharmacogenetic treatment recommendations related to this gene.
In this newly published study, pharmacogenetics of clozapine was likely examined for the first time on a biobank scale. Schizophrenia patients treated with clozapine were compared to those not using clozapine. The study observed that several well-known adverse effects of clozapine were enriched in patients who had started clozapine treatment. For example, clozapine is known to cause increased heart rate, or tachycardia. The use of beta-blockers, which slow down the heart rate, immediately became more
common following the initiation of clozapine. Among elderly patients treated with clozapine, more than 75% used beta-blockers, compared to about 60% of patients treated with medications other than clozapine or olanzapine.
Clozapine lowers the seizure threshold, and 80% of clozapine patients used antiepileptic drugs by the age of 80. The most well-known side effect of clozapine is neutropenia, but the study also found that clozapine increases the risk of pneumonia and milder respiratory infections. Reduced activity
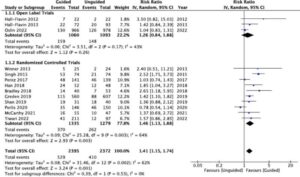
of CYP1A2 was associated with an elevated risk of pneumonia. Among individuals with low activity, the incidence of pneumonia was as high as 45%, compared to 23% in those with normal activity.
As Abomics has long included the CYP1A2 gene in its pharmacogenetic panel, the additional information provided by this study can also benefit patients who have already undergone testing. The evidence level of gene-drug interactions is continuously monitored, and it is updated as new research data becomes available.
Source: https://www.psychiatryonline.org/doi/abs/10.1176/appi.ajp.20230744?af=R